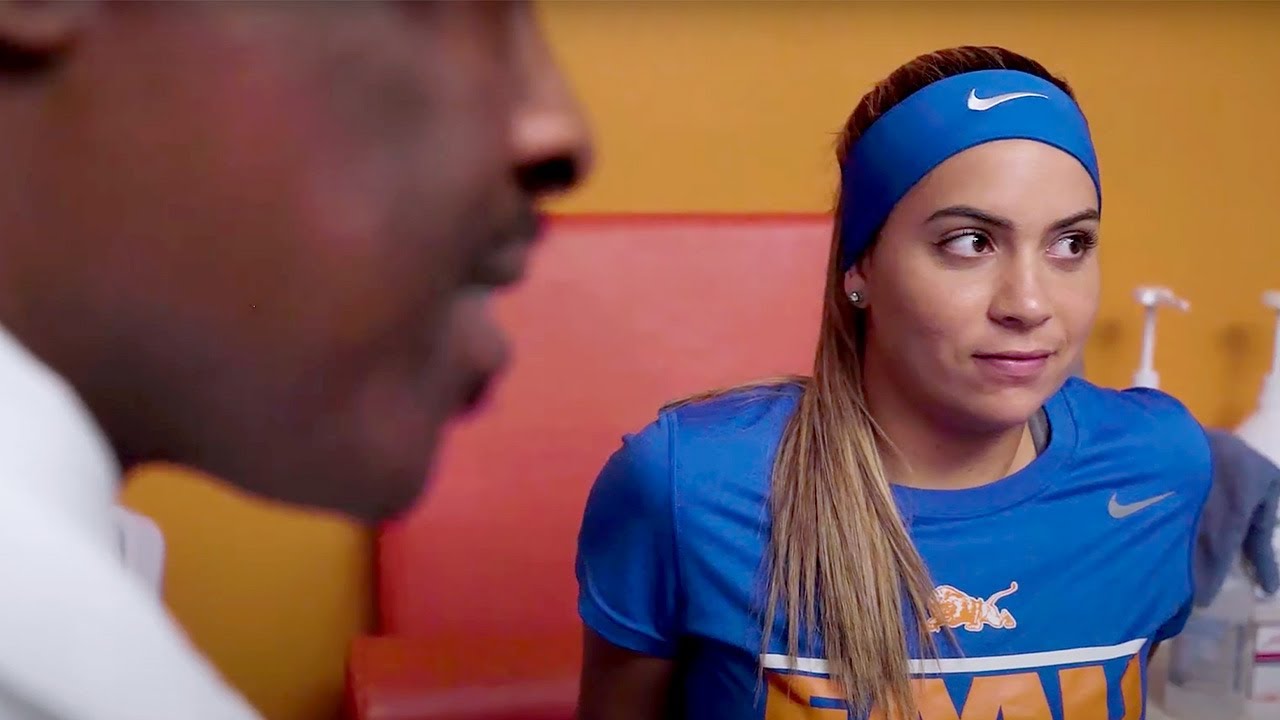Orthopedics
Explore Our Orthopaedic Services
Call us for more information or to schedule an appointment
954-265-7700It can be frustrating when an orthopaedic injury or condition keeps you from doing the activities you love. But with personalized care from an expert team, you can get back in the game. People throughout South Florida turn to Memorial Healthcare System to get specialized orthopaedic surgery and treatments for bone, joint and muscle care.
Our experienced team of orthopaedic surgeons offer advanced diagnosis, customized physical therapy and rehabilitation services, and outpatient treatment–including injections, minimally invasive procedures, and joint replacement surgery–for a variety of orthopaedic conditions.
Why Choose Memorial for Your Orthopaedic Care?
Our board-certified orthopaedic surgeons and their teams provide specialized services to diagnose and treat adult patients for all types of conditions and injuries that affect the bones, joints, muscles, tendons and ligaments. Whether you have a chronic condition, a sports injury or have been in an accident, our team provides a personalized treatment plan using the least invasive options for safe, effective care.
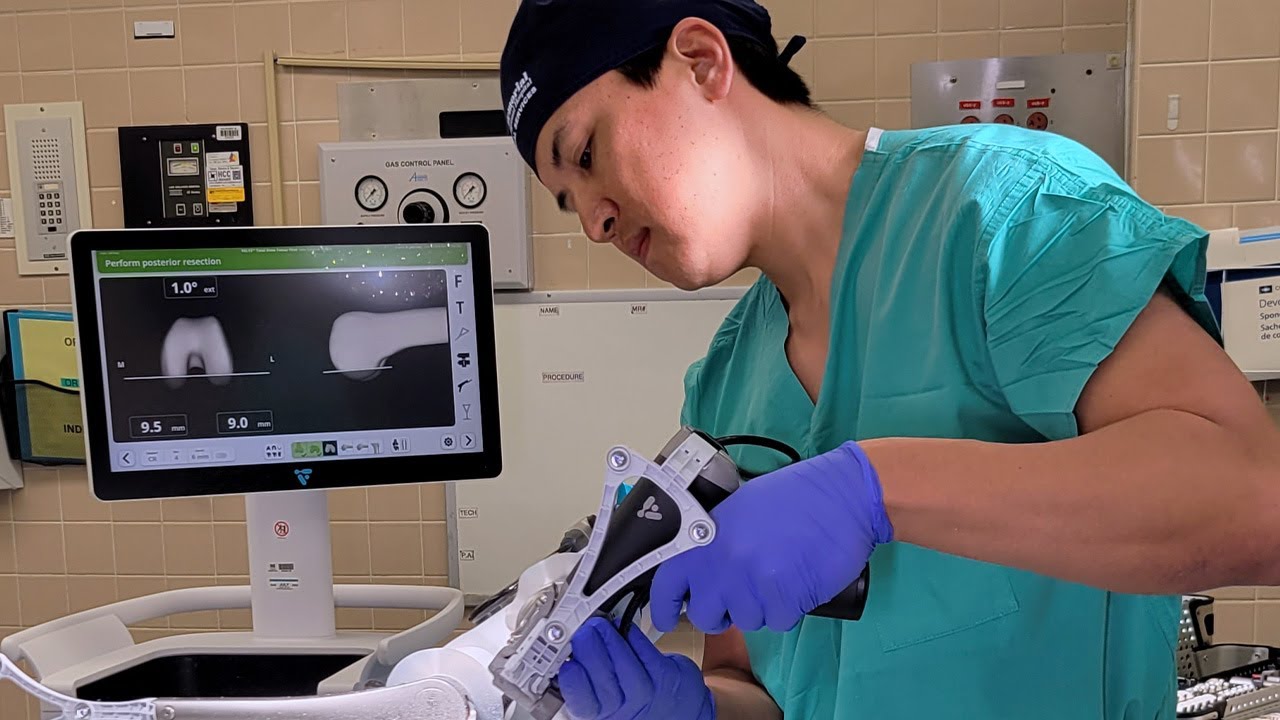
Our highly trained orthopaedic surgeons have expertise in the latest techniques for orthopaedic, trauma and joint replacement surgery. We’re particularly skilled in:
- Advanced surgical procedures to repair complex fractures
- Minimally invasive anterior hip replacement
- Arthroscopy surgery to repair a number of joint injuries and conditions
Learn more about our advanced joint replacement surgery and services.
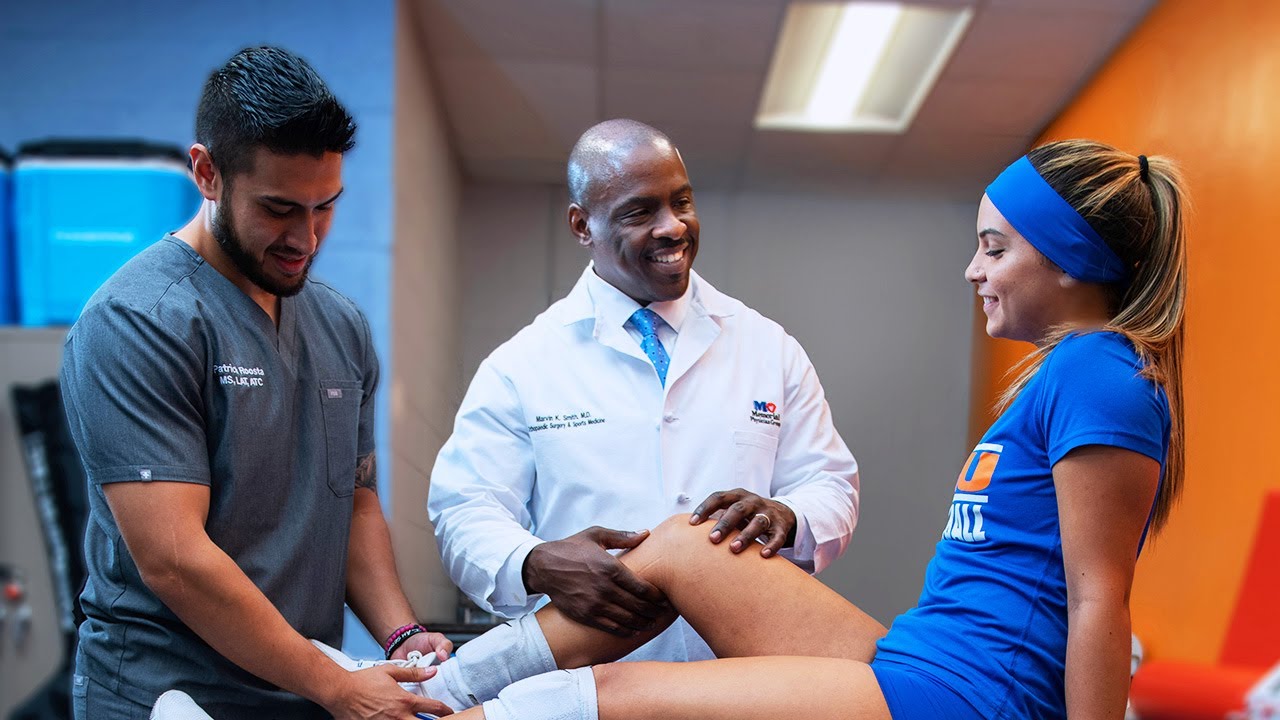
Memorial Orthopaedic Surgery & Sports Medicine Center is the first of its kind in Broward and Palm Beach Counties. You’ll find:
- Specialists in sports medicine, orthopaedics, primary care, and rehab and physical therapy, all in one program
- Doctors and surgeons with fellowship training and board certifications in sports medicine and related specialties
- Advanced services and the latest treatments for athletes at any level and people of any age who want to stay active
Learn more about the Orthopaedic Surgery & Sports Medicine Center.
Memorial Regional Hospital is one of only three Level I Trauma Centers in South Florida and the only Level 1 Trauma Center in Broward and Palm Beach Counties certified by the American College of Surgeons. Our orthopaedic surgeons are on call 24/7 to respond to emergencies.
We provide the highest level of care for people with orthopaedic trauma from traffic accidents, falls, workplace accidents and sports injuries.
Learn more about orthopaedic trauma care at Memorial.
We use conservative treatments whenever possible. Our wide range of nonsurgical options includes physical therapy and injections for joint pain.
If you need surgery, we often perform arthroscopy. This minimally invasive procedure requires only a few small incisions, decreasing pain and shortening recovery time.
Learn more about nonsurgical treatment options.
Our orthopaedic team begins with a thorough evaluation, using the latest technologies to accurately diagnose injuries and disorders. We work with specialists across Memorial Healthcare System to coordinate care for any other conditions you may have. Our integrated physical therapy services help you regain your strength and function as you recover after surgery or injury.
Memorial’s trusted orthopaedic surgery team also performs outpatient orthopaedic surgery in Ft. Lauderdale.
Our Orthopedic Surgical Services
Our Sports Medicine Services
Call us for more information or to schedule an appointment
954-265-7700