How is Arrhythmia Diagnosed
March 23, 2023
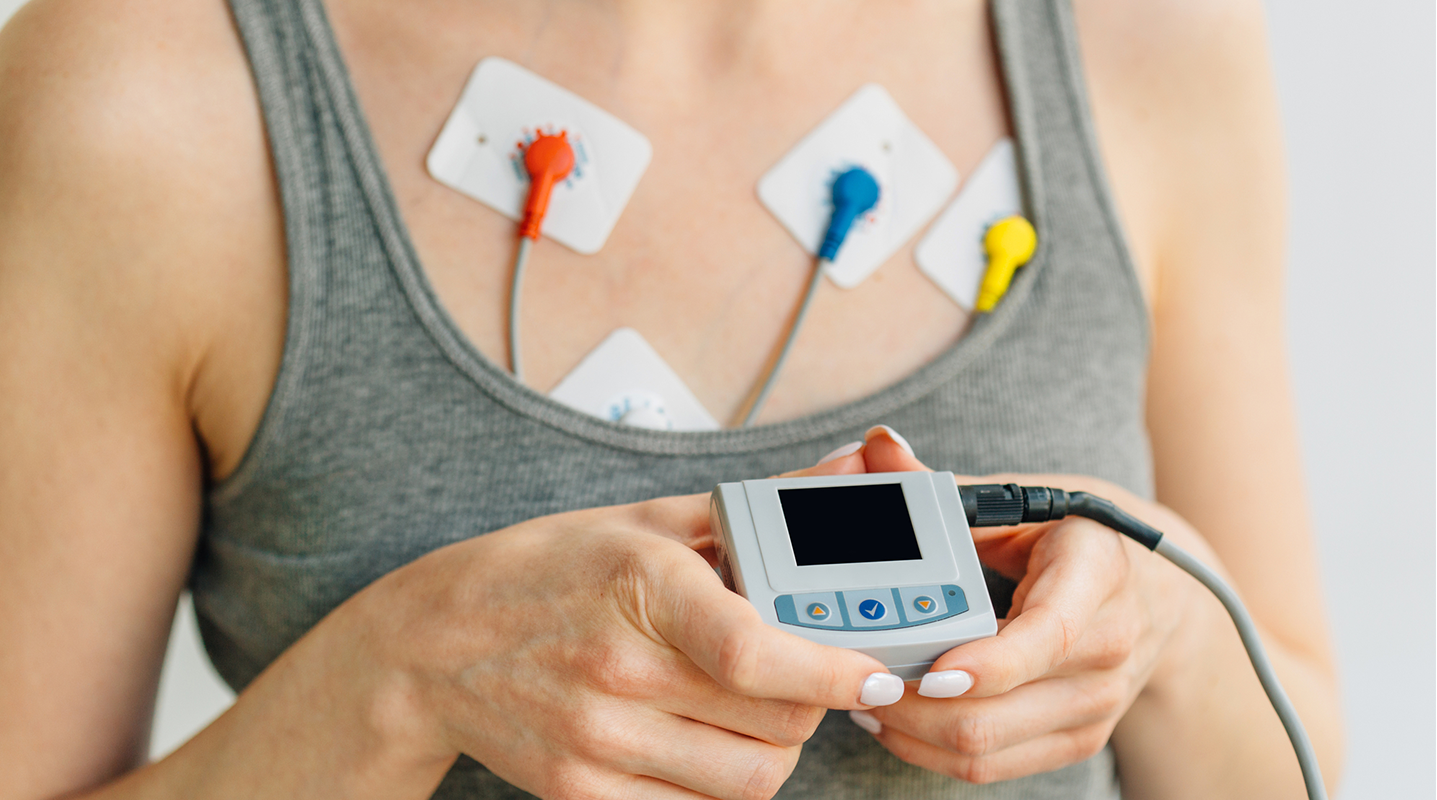
It can be surprising to learn that you have an irregular heartbeat (arrhythmia), especially if you haven’t had palpitations. But finding out your heart is misfiring is just the first step in figuring out what’s happening. There are several types of arrhythmias ranging from harmless to severe. Getting a complete work-up for a heart arrhythmia diagnosis is essential for knowing how to proceed.
How do doctors diagnose an arrhythmia? First, your primary care provider (PCP) will run some initial tests and likely refer you to a cardiologist. Then you’ll go through more diagnostic testing. Depending on your test results and diagnosis, your cardiologist may treat your arrhythmia or refer you to an electrophysiologist (EP), a doctor that specializes in diagnosing and treating abnormal heart rhythms, for further care. The good news: Healthcare providers can almost always pinpoint the type of arrhythmia you have during the diagnostic process.
Diagnostic Tests for AFib and Other Arrhythmias
The initial step in diagnosing an arrhythmia starts with a physical exam by your PCP. They will ask about your medical history, symptoms and lifestyle habits. They may also run blood tests to check for electrolyte imbalances or a thyroid disorder. Both can cause an irregular heartbeat.
There are several other tests to determine if you have the most common arrhythmia — atrial fibrillation (AFib) — or another type of abnormal heartbeat. You may need to have a number of tests, depending on how challenging your arrhythmia is to diagnose. Tests include:
Electrocardiogram (ECG or EKG)
An electrocardiogram records your heart’s electrical activity. For the test, your provider attaches electrodes to your chest to track your heart’s rhythm. An EKG can be done at rest or while exercising on a treadmill or stationary bike (stress test).
Monitoring devices
An EKG performed in a provider’s office gives a brief snapshot of your heart’s electrical activity. During the test, your heart may not show irregular beats. That’s why providers often recommend a monitoring device, which is a portable EKG you can use at home. There are a few different options:
Holter monitor
You wear this portable, battery-operated device under your clothes. The Holter monitor continually records your heart’s rhythm while you go about your daily activities.
“Even if you have data from a wearable device, like a smartwatch, that’s just the beginning of the diagnosis,” says Daniel Benhayon Lanes, MD, an electrophysiologist (EP) at Memorial Cardiac and Vascular Institute. “We still use a traditional monitor like a Holter monitor to find out how often you have arrhythmia episodes. The consumer wearables just tell you whether you have it.”
Cardiac event monitor
Unlike a Holter monitor, a cardiac event monitor only takes readings when you turn the monitor on while you have symptoms, like feeling faint or lightheaded, so that it can record your heart’s electrical activity. This helps your healthcare provider decide if your symptoms are related to heart rhythm changes.
Implantable loop recorder
An implantable loop recorder is a long-term option for tracking your heart’s activity. It’s a chip that’s placed under the skin atop your chest. If you wear a Holter monitor for 30 days and it doesn’t find anything, your provider may recommend you wear an implantable device for up to three years.
“It’s especially helpful if someone has a stroke for no obvious reason,” says Dr. Lanes. “It’s highly possible that in those situations, the person has an undiagnosed arrhythmia that caused the stroke. Arrhythmias can cause clots to form in the heart. Clots can dislodge, travel to the brain and block blood flow.”
The implantable loop recorder detects abnormalities and sends data to a remote patient monitoring center.
“At Memorial, we regularly check the data, and alerts are sent to the right teams at the right times,” notes Dr. Lanes. “The data helps to know if there’s an urgent situation or if we need to change the course of treatment.”
Imaging tests
If you’re having heart problems, your provider will likely want to look at your heart. Imaging tests show whether your heart structure is normal. You may have one or more imaging tests, such as:
- Echocardiogram, an ultrasound of the heart, which uses sound waves to create images of your heart as it beats.
- Cardiac CT scan, a series of X-ray images put together to create high-resolution, 3D pictures of your heart.
- Cardiac MRI, which produces highly detailed images of your heart using magnetic fields and radio waves.
Genetic testing
Some inherited disorders cause arrhythmias. You may need genetic testing if your provider suspects you have one of these conditions. The test requires a blood sample and checks to see if you have a gene linked to certain arrhythmias.
If these test don’t find an arrhythmia, your doctor may trigger an arrhythmia using one of the following test to be able to study your abnormal heartbeat while it’s happening.
Stress test
This test attempts to trigger an arrhythmia by monitoring how much stress your heart can manage while exercising (i.e., walking or jogging on a treadmill or pedaling a stationary bike). If these exercises are not an option, medication may be given to increase your heart rate.
Esophageal electrophysiologic procedure
This procedure involves inserting a thin tube (catheter) in the nostril down to the esophagus (tube that connects the throat to the stomach), where it takes an EKG reading. This test is more accurate than a traditional EKG because the catheter is positioned closer to the heart.
The procedure can trigger an arrhythmia. If this happens, your healthcare provider can use it as an opportunity to test which medications will work best to regulate your heart’s rhythm.
Electrophysiology study (EPS)
An electrophysiology study is a specialized test performed by an EP to find out where in the heart the arrhythmia begins and to guide treatment. You’re given medication to help you relax and feel sleepy, but you won’t be asleep. Next, the doctor inserts a sheath through a blood vessel (usually in the leg, arm or neck) to your heart. Several thin wires (electrodes) are guided through the sheath to different areas of your heart. Your heart receives electric pulses to trigger an arrhythmia so your doctor can study it.
Tilt table testing
For some people, like those with postural orthostatic tachycardia syndrome (POTS), a change in position can cause fainting. The tilt table test replicates this situation to study what happens to your heart when you switch positions. For the test, you lie down on a table and get strapped in. A healthcare provider attaches a blood pressure cuff to your arm and electrodes to your chest for an EKG. The provider gradually tilts the table up. The test measures your heart rate and blood pressure as the table rises.
Schedule an Appointment for Heart and Vascular Services
If you have an irregular heartbeat, it’s important to get further testing. Learn more about heart and vascular services at Memorial Cardiac and Vascular Institute. To schedule an appointment with a cardiologist, electrophysiologist or vascular specialist at Memorial, call 1-855-400-6284.



